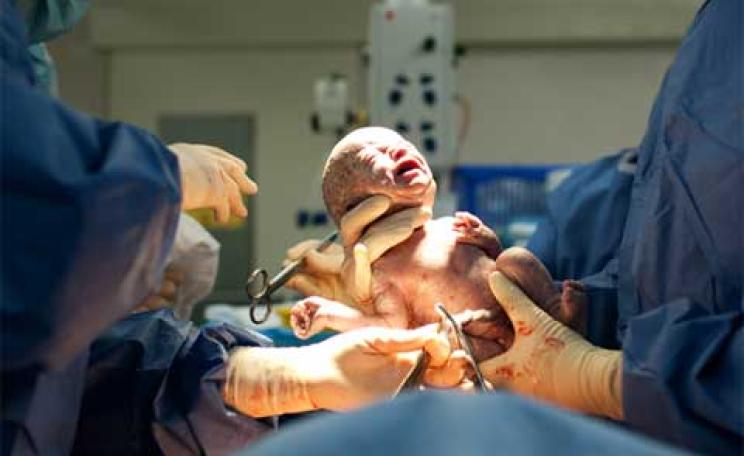
A healthy woman walks into her doctor's office. She says ‘Doctor, I'd like to have major abdominal surgery, please.'
In most medical settings a doctor would balk at the idea and be very clear about the ethics of cutting open a healthy body for no good reason. But this woman is pregnant and so the doctor agrees it's probably for the best.
What both the woman and the doctor have in common is they make their decisions in a culture of fear.
Caesareans on demand and for no medical reason are still quite rare - according to recent figures in the region of 1.7 per cent of all births in the UK. In the US the rate is around 2.5 per cent.
But the figures are rising and are symbolic of an increasingly utilitarian and technocratic approach to birth which has seen rates of interventions in labour - everything from drugs to speed it up, to instrumental (forceps and vacuum extraction) deliveries, to caesarean operations - becoming more common.
The latter is a cause for real concern. While the non-medically justifiable caesarean operation may still be rare, the rate as a whole is exploding. Today 24 per cent of all births in the UK and 34 per cent in the US are by caesarean, compared to a World Health Organization recommended safe and appropriate rate of 10-15 per cent. The rise is the result of both fear and the unnecessary interventions in the birth process that arise from that fear.
Birth gone wrong
When a healthy woman ends up with a caesarean, whether on demand or as a result of an ‘emergency', you can guarantee that a lot of things have gone wrong for her along the way. Fear of birth for instance has been linked to pre-existing depression and anxiety, to previous bad birth experiences, to negative self-image, lack of support from family and partners, and to lack of good ante-natal education and to lack of solid midwifery care.
Any and all of these things can lead to growing and irrational fear of the process of birth.
This is why clinical guidelines laid down by the UK's National Institute of Clinical Excellence (NICE) advise against caesareans on demand. Instead they suggest that women who express extreme anxiety about giving birth should be referred for psychological counselling and support.
Under the knife
That's because surgery carries real risks. It also does not guarantee a satisfying birth experience because it does not address fear or things that provoke it, a fear which campaigners say is growing.
'The calls we are getting do suggest that women are becoming more afraid of birth,' says campaigner Beverly Beech, Chair of the Association for Improvements in the Maternity Services.
But the fears, she says, are becoming more specific with women convinced that normal physiological birth will cause their wombs to rupture, their vaginas to rip apart and anal sphincters to prolapse - not to mention the ruination of their sex lives. Under the weight of such fear a ‘quick cut' is seen as the best way to avoid all the ‘pain and mess' of birth.
‘Very often they have seen something on TV or read something in a newspaper that has been hyped up or misinterpreted or frankly is just a lie that's been spun to make the story more dramatic and controversial' she says.
But far from being up and back at work within a few days the quick cut option can lead to weeks of pain, the inability to pick up or breastfeed your baby easily and the potential serious long term adverse effects, such as excessive bleeding, blood clots, surgical injury, increased risk of placenta praevia, infection and internal damage that could endanger the normal progress of any further pregnancies and prevents any future normal births.
 Looking for problems
Looking for problems
The vast majority of pregnancies are normal and healthy and regardless of what type of birth she may be angling for, every woman is looking for a good birth experience.
Nevertheless, feelings of anxiety are natural to pregnancy - as natural as they are to any other major life transition. A woman might fear miscarriage, fear for the baby's well-being, fear for her ability to cope with labour or parenthood, fear her partner's reaction to her labour.
It's fair to say that most women perceive antenatal screening as a good way of addressing these anxieties. But routine testing, whether it's the seemingly trivial ritual of weighing a woman or the more invasive amniocentesis, often ends up amplifying fear rather than assuaging it.
Antenatal care takes place in hospitals and clinics, places where sick people go. The atmosphere in which most ante-natal testing is done, with its emphasis on illness and abnormality, can provoke enormous anxiety and loss of confidence among women.
The unhelpful routines of the hospital environment can also breed fear in caregivers, prompting them to intervene routinely and unnecessarily. By the time a woman is ready to give birth she may have all but lost confidence in her ability to do the job she was built for.
TV terrorism
It was Winston Churchill who once said that there was nothing so exhilarating as being shot at and missed.
A woman with a strong sense of self and good social support can usually weather the trial of antenatal care. But the media barrage of birth-as-a-bullet-with-your-name-on-it stories is harder to withstand.
Images of birth on TV and films have existed for generations, but it is only recently that ‘reality' TV has turned its focus on the hospital birth machine. While a TV drama such as Call the Midwife may still be considered entertainment, a reality show such as One Born Every Minute carries much more influence in its message.
We watch these shows at our peril because although they contain graphic images of ‘how it is' they lack any commentary to help us understand ‘why it is'.
Decades of social science research shows that such programmes act like marketing campaigns for hospitalised birth and do little more than breed fear and ignorance.
A battleground
Sarah Davies Senior midwifery lecturer at the University of Salford, School of Nursing, Midwifery and Social Work, is very clear about their toxic influence: ‘Anybody watching could be forgiven for thinking ‘I don't want to give birth like that'. Inevitably the women and their support partners are portrayed as frightened and out of control. The women are always on their backs - something that is frankly inexcusable under so-called midwifery care. They are hooked up to monitors which draw more of the midwife's focus and attention than the woman herself. They are told when to push, when not to push, what drugs to take.' What is more says Davies such programmes inevitably portray birth as a battle between mother and baby ‘as if the two were in opposition'. Certainly no mention is made of the benefits of birth for the baby, such as preparing its lungs for life in the air.
Beverley Beech, Chair of the Association for Improvements in the Maternity Services agrees: ‘In these programmes the woman's needs, her comfort, her sense of security and privacy is completely ignored and of course when it all goes wrong the obstetrician is invariably portrayed as the knight in shining armour who sweeps in to save the day. There is never any comment on how every aspect of the woman's care up to that point caused the "emergency" in the first place.'
The cascade of interventions
The rubric is well proven in the medical literature. Induction = increased pain = epidural = slowed labour, uncoordinated contractions = more attempts at induction = more pain relief = fetal distress and maternal exhaustion = caesarean. And these days caesarean = infection with antibiotic resistant MRSA.
Indeed infection is still an aspect of the post-caesarean operation which is under-explored and under-reported. Caesareans classically carry a 5 to 20-fold risk of infection over vaginal delivery with between 4-29 per cent of women experiencing an infection after a caesarean. Likewise, endometritis (infection of the uterus) is estimated to occur up to ten times more frequently following a surgical delivery.
 The baby is at higher risk of an MRSA infection too. In a 2010 study, researchers found that babies delivered vaginally had bacterial communities resembling their mother's vaginal bacteria, and generally considered protective. Caesarean operation newborns, however, carried bacteria that was more common on the skin, such as MRSA. The difference may explain why babies born surgically can be more susceptible to certain illnesses, allergies and asthma than newborns born vaginally. Previous studies have also demonstrated this.
The baby is at higher risk of an MRSA infection too. In a 2010 study, researchers found that babies delivered vaginally had bacterial communities resembling their mother's vaginal bacteria, and generally considered protective. Caesarean operation newborns, however, carried bacteria that was more common on the skin, such as MRSA. The difference may explain why babies born surgically can be more susceptible to certain illnesses, allergies and asthma than newborns born vaginally. Previous studies have also demonstrated this.
As important as what we see is what we don't see - the hidden timetables that only ‘allow' a woman to labour for so long before intervening to speed things up. These timetables, or partograms, are not based on science, but on a bureaucratic need to get the women in and out of the system as quickly as possible.
All such interventions are the medical equivalent of pulling the bottom block from a Jenga tower and then watching the whole thing come crashing down.
A safe place to give birth
Undoubtedly the maternity care system lets women down. According to Davies the UK has one of the most progressive policies on maternity care, but the gap between policy and practice is frighteningly wide: ‘In the UK, in theory, all women should have one-to-one care, all women should have access to water for pain relief, all women should have the option of a home birth with a skilled midwife. All these options are central to a community-based, woman-focused ethos of care. But in reality local hospitals and midwife-led maternity units are being closed down and women are more and more being shunted into large centralised hospitals where there is a culture of medical management and intervention that makes the hospital a less safe place to give birth.'
That larger centralised hospitals are the least safe place to give birth was underscored in 2011 in the National Perinatal Epidemiology Unit's Birthplace Study, which showed that today the fewest number of women give birth in the safest places of all - stand alone midwifery units and at home.
Says Beech: ‘We know that the midwife is the only practitioner skilled enough to safely facilitate normal birth, but we do not invest in our midwives. We insist midwifery students complete their education in hospitals where the experience turns them into obstetric nurses more concerned with schedules and paperwork than supporting women. Midwives who work outside the hospital system can retain their focus on supporting women, but we do not support these midwives. Now with their insurance premiums rising many are being forced out of business and with them women's choice of an independent midwife'
The rise in fear of birth, she notes, has also paralleled the loss of our midwives and midwifery units.
A responsibility revolution?
But, women also let themselves down.
The inescapable truth is that the modern history of pregnancy and birth is in part a history of women's capitulation - to doctor/hero myth, to the idea that their bodies are dysfunctional, to the idea of the baby as a passenger, neither affecting or being affected by the process, and to the idea that birth matters less than everything that comes before or after it.
This is not a popular point of view amongst childbirth campaigners who tend towards seeing women as victims of the system.
Victims or not, the ‘responsibility revolution' which demands that we understand our place in the larger scheme of things and the short and long-term consequences of our actions, seems to have passed many childbearing women by. The same woman who might spend extra time reading labels on the food and cosmetics she buys, may spend little or no time reading up on the consequences of medicalised birth.
Occupy birth
In part the natural and active birth movements of the 80's and 90s have stalled in recent years due to lack of compelling public figureheads to match those of Janet Balaskas, founder of the Active Birth Movement and the indomitable birth guru and social scientist Sheila Kitzinger. We are also missing the language and the sensitive analysis of doctors like Michel Odent who spoke of birth as an act of love, rather than a hi-tech race to the finish line.
Instead of a trend towards a confident and joyful ‘occupying ‘of their own birth experiences, what we are left with is an assembly line vision of birth that is a little too close to Huxley's Brave New World for comfort. In the face of such lack it's not the rising tide of caesareans that should shock us as much as the number of women who still manage to avoid the knife.
Even in this technocratic age birth, a 100% natural process, has stubbornly refused to be completely mechanised, with the vast majority of women still hopeful for a normal, happy birth experience. The question is how do we help maintain that positive aspiration?
Says Davies ‘Women don't hear enough positive things about birth. Women need positive vibes and feedback and not lots of scare stories. We need to find a midpoint between what is perceived as the kind of brutal "for your own good honesty" we so often see in the media and the sometimes unrealistic stories about orgasmic birth.
‘Birth is not just one experience but many, as varied as the women participating in it. The idea of controlling it is ridiculous, but what we can do is create environments where women feel cared for and acknowledged, where birth is seen as a relevant and integral part of life's journey and not just a lifestyle choice and where watchful waiting takes precedence over active intervention. If women want to feel safe that is where it will begin.'
Pat Thomas is the former editor of the Ecologist and the author of several books on pregnancy & birth including Your Birth Rights, Alternative Therapies for Pregnancy & Birth and Every Birth is Different.
If you want a normal birth, start here...
AIMS - The Association for Improvements in the Maternity Services
50 years of experience helping women achieve normal birth, web and print resources and a comprehensive list of links to supportive organisations. For the US see: Alliance for the Improvement of Maternity Services - AIMS USA
Active Birth Centre
Providing information and products to help parents make informed choices. Specialists in waterbirth and Active Birth ante-natal classes.
BirthChoiceUK
Independent website helping women in the UK to choose where to give birth. Provides comparative statistics on interventions and outcomes in different hospitals.
One World Birth
Online video community focussing on the state of birth around the world today with contributions from experts like Sheila Kitzinger, Ina May Gaskin. Michel Odent and many others.
The Business of Being Born
Home of the 2008 film, expanded to a 4 part series in 2011, by TV presenter Ricki Lake. Part expose of the corporatisation of birth, part moving and inspiring plea for normal birth. Available on iTunes.
Caesarean Birth and VBAC Information
Information about caesarean birth and VBAC. Articles, reading list, birth stories, scar pictures and more.
Doula UK
A volunteer organisation run by Doulas, provides information about Doula and contact details of practicing Doulas.
National Childbirth Trust
Antenatal education and postnatal support for UK parents.
| READ MORE... | |
 |
NEWS ANALYSIS Maternity special Labour of love: the demise of traditional midwifery Women-centred maternity care through midwifery is in danger of extinction, replaced by a medical model that treats birth as an illness. Birth is an act of love, not one of fear and loathing, so what are the consequences? Matilda Lee reports |
 |
HOW TO MAKE A DIFFERENCE Maternity special Flash 'em: how breastfeeding got political An exclusive interview with Claire Jones-Hughes - the woman behind Brighton’s now famous breastfeeding flash mob. By Matilda Lee |
 |
HOW TO MAKE A DIFFERENCE Maternity special Top 10 myths about new parenthood Worried your life, your marriage, your baby or your body isn't 'normal'? Don't fall foul of the myths of parenting |
 |
GREEN LIVING Maternity special Top 10...tips for a natural labour Whether it’s raspberry leaf tea or a spot of stretching, pregnancy massage specialist Holly Jeffery suggests some all-natural ways to keep labour pain at bay |
 |
COMMENT Maternity special Anatomy of a C-section: they save lives, but would you choose one? Andrew Wasley watched his partner endure two invasive births, one elective, the other life saving |