m
Scientists and regulators have been debating the use of glyphosate and other chemical pesticides for years. Expert assessors have made claims for and against glyphosate's potential to cause cancer in humans without arriving at a satisfactory consensus and, unsurprisingly, the European Union's reauthorisation of glyphosate in 2017 resulted in calls for an overhaul of the regulatory process.
Subsequent hearings conducted by the European Parliament's Special Committee on the Union Authorisation Procedure for Pesticides covered important topics but failed to identify the deeper, more insidious cause of regulatory uncertainty: reliance on the wrong species.
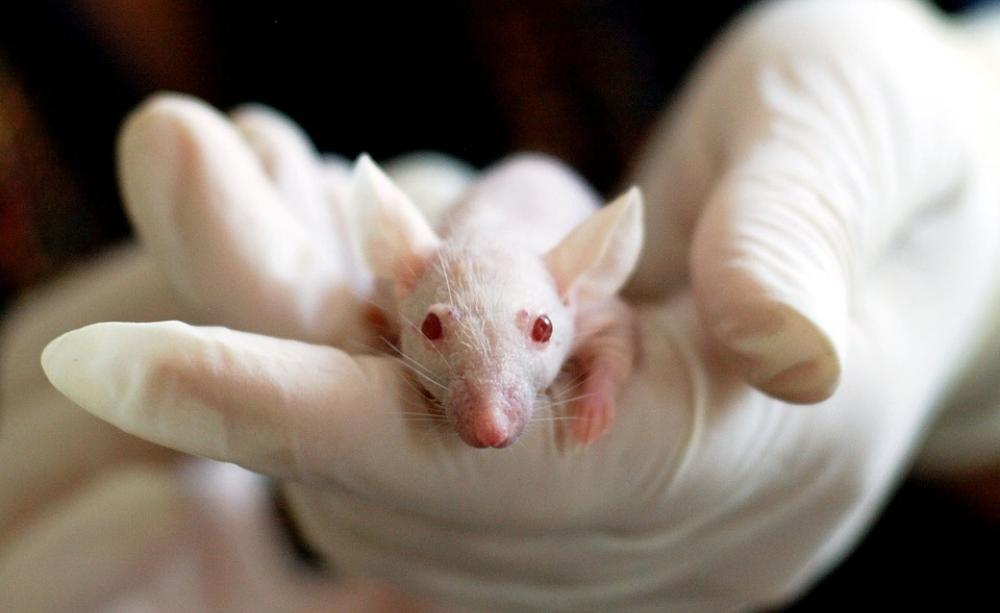
Thousands of rats, dogs, mice, and rabbits have suffered and died in tests for the "safety" assessment of glyphosate. Yet, after decades of testing and retesting, uncertainty surrounding the potential toxicity of the substance – which is widely used in agricultural and consumer products – seems, if anything, to have intensified.
Unreliable tests
Regulators rely heavily on the two-year rodent cancer bioassay to decide whether a chemical will cause cancer in humans.
The test, which was globally adopted as a standardised protocol in 1981, requires hundreds of rats and/or mice and is notorious for producing variable results of questionable relevance to human health.
As many scientific experts will confirm, substances known to cause cancer in humans often fail to do so when tested in rats and mice, and the opposite is also true: one study showed that out of 20 known non-carcinogens in humans, 19 were found to be carcinogenic in other animals.
To assess the human carcinogenicity of glyphosate, international evaluators looked at fourteen separate rodent cancer tests (eight using rats and six using mice). More than 3,500 animals were used, but not a single experiment produced the same results when repeated. EU risk assessors studied additional unpublished test data, meaning the total number of tests conducted is even higher, yet confidence in the regulatory outcome is at an all-time low.
Under today's validation standards, the rodent cancer bioassay wouldn't stand up to the scientific scrutiny that is required of new testing strategies under development.
Repeated mistakes
When studies yield questionable and inconsistent outcomes, there has been a tendency – especially with controversial chemicals such as glyphosate – to ignore the problems associated with testing on animals and, astonishingly, to call for more animal testing.
In addition to causing yet more animal suffering, uncertainty leads to delays in regulatory decisions for years or even decades.
According to the president of the German Federal Institute for Risk Assessment, for just seven of the required toxicology tests used to assess glyphosate, over 100 separate studies have been conducted and at least 31,000 animals have been killed.
Yet, in addition to being unreliable predictors of adverse health effects in humans, the data produced from these laboratory tests are difficult to extrapolate to real-life human exposure.
There is little doubt that relying on flawed animal tests is hazardous to humans, and the problem won't be solved by throwing more money at irrelevant tests on animals.
Animal suffering
One rodent cancer bioassay typically uses more than 400 animals.
It begins as soon as possible after the rat or mouse pups are weaned. Usually, they're forced to ingest chemicals by gavage (a procedure that involves forcing a tube down their throats).
The substances can produce side effects such as painful, long-term tumour growth as well as lethargy, nausea, tremors, and convulsions. The animals undergo daily dosing for up to two years before being killed and dissected.
For each individual animal used in these experiments, pain, suffering, and death are certain. If the goal is to protect human health, regulators and researchers must acknowledge the limitations of these studies and instead rely on data collected using human-relevantmethods.
Superior methods
Fortunately, a paradigm shift toward human-relevant, non-animal test methods is already underway. There are myriad human cell-based techniques and computational models for predicting many adverse health effects, such as local effects on the skin and eyes.
Assessing chemical carcinogenicity is complex, but scientists are rapidly establishing new strategies for identifying potential human carcinogens.
To screen effectively for carcinogens, some researchers are using human tissues to find early-stage cancer markers. Others are developing advanced computational models using artificial intelligence to learn about carcinogenic chemical signatures.
In addition, large, long-term human population studies, such as the Agricultural Health Study, are collecting decades of data to assess the correlation between pesticide application and cancer.
This new, human-relevant technology is bringing us closer to replacing flawed animal tests in order to provide reliable predictions for chemical safety and better protection of human health.
Regulatory shift
Following work carried out by its special committee, the European Parliament has recommended strengthening the regulation of pesticides, improving access to information, and promoting "low-risk" alternatives made from naturally occurring substances.
Importantly, the Parliament recognised the flaws inherent in using animals to predict effects in humans as well as the need for data sharing in order to reduce animal testing and accelerate the development of human-relevant tests.
However, for new methods to be accepted by regulatory authorities, there must be a collective effort by all stakeholders, including manufacturers, regulators, and scientists, to work together to improve the current battery of non-animal tests. The focus must be on human-relevant data.
This Author
Emily McIvor is a science policy adviser for People for the Ethical Treatment of Animals Foundation and has more than 20 years of experience of working on EU policy.