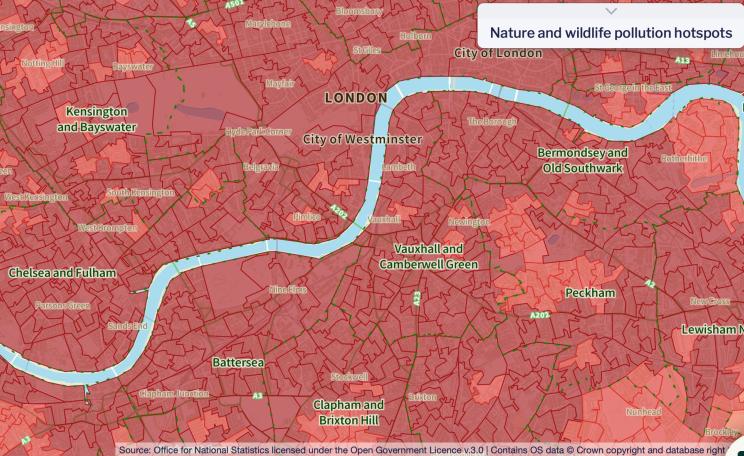
With current trends, the amount of pharmaceutical effluence leaching into waterways could increase by two-thirds before mid-century, according to a 2018 study by the Delft Institute for Water Education.
Photographs accompanying stories about the climate emergency or the nature crisis, the disastrous impacts of human activity on our poor, overstretched planet, will usually be an industrial smokestack or a crowded highway. You're unlikely to see an image of a hospital.
But in the midst of the environmental crisis that we face – and pressing issues where human health and environment meet, such as antibiotic resistance and Covid-19 – we need to think about the impacts of our healthcare system on our environment.
That’s also true of veterinary medicines. The Medicines and Medical Devices Bill now before the House of Lords acknowledges this connection, addressing - for example - the impact of anthelmintics on insect populations. What’s lacking is an environmental focus in the human medicines and medical devices sections.
Harm
Of course people will say “human health always has to be the top priority”. But this is not a case of saying we have to weigh health benefits against environmental ones. This is not a case of either/or.
We hear almost daily now a new report on the health impacts of air pollution, and the pervasiveness of plastics in our food, our water, our lives. That's to say nothing of Covid-19 and antimicrobial resistance. Our healthcare systems have impact on all of these.
This is fast-growing area of medical concern and engagement. A project under the EU’s Innovative Medicines Initiative is aiming to develop tools to screen environmental properties earlier in drug development.
Stockholm County Council grades medicines on their environmental effects, and doctors are able to prescribe a less harmful drug where the option exists. If the UK Government wants to be world-leading, well that is the standard to get ahead of.
With current trends, the amount of pharmaceutical effluence leaching into waterways could increase by two-thirds before mid-century, according to a 2018 study by the Delft Institute for Water Education.
And then of course there’s the greenhouse gas impacts of medicines and medical devices. The World Bank estimates that the healthcare sector makes up approximately 5 percent of global carbon emissions and the Sustainable Development Unit of the NHS estimates 30 percent of its emissions can be linked to pharmaceuticals and medical devices.
Urgency
Overall what we are talking about here is “green pharmacy”, which recognises the potential for designing new drugs that are less harmful for the environment – and I’m arguing that the expectation of this approach should be built into the Medicines and Medical Devices Bill.
I know that it is of concern to many in the healthcare community, having chaired a recent Westminster Forum event on sustainability and healthcare. Excellent work being done by Health Care Without Harm.
This is an urgent and growing issue now. The context in which this Bill comes before us is an ageing demographic, the rise of chronic health conditions in our deeply unhealthy society and the advent of so-called lifestyle drugs have been the key drivers of increased pharmaceutical medicine use.
Rates of use of medicines from antidepressants to statins are leaping ever upward, sometimes in ways that lead to questions about alternative, non-medical, interventions.
Optimism?
Critics of the pharmaceutical industry have highlighted how a “culture of optimism” is generated around the value of new drugs, which increases the demand for such treatments while simultaneously exaggerating their benefits (and currently not counting their flow-on costs, including environmental).
There are three main ways drugs can enter the environment: by passing through the body, by being disposed of in waste, and through the manufacturing process.
In most of 160 sewage treatment works studied by UK Water Industry Research in 2014, several common drugs were present in the final effluent in concentrations high enough to affect ecosystems. With current trends, the amount of pharmaceutical effluence leaching into waterways could increase by two-thirds before mid-century, according to a 2018 study by the Delft Institute for Water Education.
It is worth noting that globally over half of all medicines are prescribed, dispensed or sold inappropriately, and that half of all patients fail to take them as directed. Research undertaken in Germany found that up to 16,000 tons of pharmaceuticals were disposed of annually from human medical care, with 60–80 percent of these drugs flushed down the toilet or placed in normal household waste.
Drug manufacturing facilities are an important source of environmental pollution, as argued in a 2018 study by the US Geological Survey. Improved sewage treatment can reduce the amount of pharmaceutical residue reaching ground and surface waters, but dealing with problem after it has been generated is not the ideal approach.
Circularity
The Bill should ensure there is consideration of the social impacts of the productions of medicines and medical devices. We might think of a medical device made from a mineral obtained by “artisan mining” in the Congo - to the great detriment of the health and wellbeing of child labourers and others there - or a drug made from a rare plant then effectively denied to an indigenous community that has relied on it for its own use.
No one is safe until everyone is safe, as many global health leaders have reminded us in the context of ebola and Covid-19. A safe and healthy world is crucial to every individual’s health.
Novo Nordisk, a global company based in Denmark, has a new environmental strategy - Circular for Zero - that aims to move from a linear economy of “take-make-dispose” to a circular economy based on three principles: design out waste and pollution, keep products and materials in use, and regenerate natural systems. That is clearly how we must organise the design, production and management of medicines and medical devices.
The debate on the Bill, including the government’s response to my contribution, can be found here.
This Author
Natalie Bennett is a Green Party peer.